The statsmodels package in Python (version 3.7.8 Python Software Foundation) was used to conduct all analyses. Among the 1,497 respondents who completed all three surveys, longitudinal analyses of the odds of incidence**** of symptoms of adverse mental or behavioral health conditions by essential worker and unpaid adult caregiver status were conducted on unweighted responses using logistic regressions to calculate unadjusted and adjusted †††† odds ratios (ORs), 95% CI, and p-values (α = 0.05). Comparisons within subgroups were evaluated using Poisson regressions with robust standard errors to calculate prevalence ratios, 95% confidence intervals (CIs), and p-values to evaluate statistical significance (α = 0.005 to account for multiple comparisons). §§§Īnalyses were stratified by gender, age, race/ethnicity, employment status, essential worker status, unpaid adult caregiver status, rural-urban residence classification, ¶¶¶ whether the respondent knew someone who had positive test results for SARS-CoV-2, the virus that causes COVID-19, or who had died from COVID-19, and whether the respondent was receiving treatment for diagnosed anxiety, depression, or posttraumatic stress disorder (PTSD) at the time of the survey. Respondents also reported whether they had started or increased substance use to cope with stress or emotions related to COVID-19 or seriously considered suicide in the 30 days preceding the survey. ¶¶ Symptoms of anxiety disorder and depressive disorder were assessed using the four-item Patient Health Questionnaire*** ( 4), and symptoms of a COVID-19–related TSRD were assessed using the six-item Impact of Event Scale ††† ( 5). population by gender, age, and race/ethnicity.  
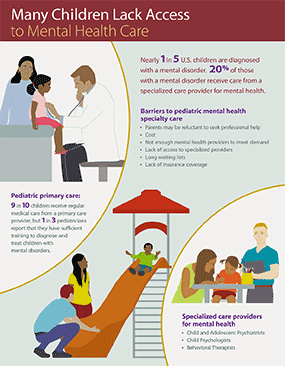
Quota sampling and survey weighting were employed to improve cohort representativeness of the U.S. Participants included 3,683 (68.1%) first-time respondents and 1,729 (31.9%) respondents who had completed a related survey during April 2–8, May 5–12, 2020, or both intervals 1,497 (27.7%) respondents participated during all three intervals ( 2, 3). Respondents were informed of the study purposes and provided electronic consent before commencement, and investigators received anonymized responses. §§ The Monash University Human Research Ethics Committee of Monash University (Melbourne, Australia) reviewed and approved the study protocol on human subjects research. Community-level intervention and prevention efforts, including health communication strategies, designed to reach these groups could help address various mental health conditions associated with the COVID-19 pandemic.ĭuring June 24–30, 2020, a total of 5,412 (54.7%) of 9,896 eligible invited adults** completed web-based surveys †† administered by Qualtrics. The percentage of respondents who reported having seriously considered suicide in the 30 days before completing the survey (10.7%) was significantly higher among respondents aged 18–24 years (25.5%), minority racial/ethnic groups (Hispanic respondents, non-Hispanic black respondents ), self-reported unpaid caregivers for adults § (30.7%), and essential workers ¶ (21.7%). 
Overall, 40.9% of respondents reported at least one adverse mental or behavioral health condition, including symptoms of anxiety disorder or depressive disorder (30.9%), symptoms of a trauma- and stressor-related disorder (TSRD) related to the pandemic † (26.3%), and having started or increased substance use to cope with stress or emotions related to COVID-19 (13.3%). To assess mental health, substance use, and suicidal ideation during the pandemic, representative panel surveys were conducted among adults aged ≥18 years across the United States during June 24–30, 2020. The coronavirus disease 2019 (COVID-19) pandemic has been associated with mental health challenges related to the morbidity and mortality caused by the disease and to mitigation activities, including the impact of physical distancing and stay-at-home orders.* Symptoms of anxiety disorder and depressive disorder increased considerably in the United States during April–June of 2020, compared with the same period in 2019 ( 1, 2).
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
